


Common Eye Problems | Diabetic Eye Disease | Retinal Detachment | Glaucoma | Eye Camp | Opticals | Medical Ethic | Diabetic Diet
Cataract Surgery - MultiFocal
Lens Implants
INFORMATION BROCHURE ON CATARACT SURGERY
This information is to help you make an informed decision about having cataract
surgery to treat your cataract.
Cataract is clouding of the eye’s natural lens. It is a natural process of
ageing. Every person gets it sooner or later. It impairs focusing of light on
the retina and hence blurs vision.
People with cataract even when wearing glasses typically have difficulty in
activities such as driving at night, recognizing colours, seeing in the distance
or reading, and sometimes frequently change their glasses.
There are no medicines with proven efficiency to prevent or treat cataract. The
only effective treatment worldwide is surgical removal of cataract and
intraocular lens implantation. Diabetes, Hypertension and other general health
problems are not a contraindication for cataract surgery. The cataract is
usually removed before it matures to avoid vision threatening complications such
as phacomorphic glaucoma ( bursting of the lens), Zonular dehiscence(breakage of
lens support mechanism) etc.
The decision to treat a cataract is reached by the eye care practitioner and the
patient together. This decision is based on the degree to which the cataract is
impairing vision and the effect of the impairment on the patients quality of
life.
Todays cataract surgery is a marvel of medical technology. At Sri Venkateswara
Nethralaya it is mostly performed as a outpatient procedure and is a very
sophisticated automated process(PHACOEMULSIFICATION).
In this procedure, the clouded lens is extracted by fragmenting it into tiny
pieces with ultrasound energy( Phacoemulsification) and aspirated out with a
suction device.
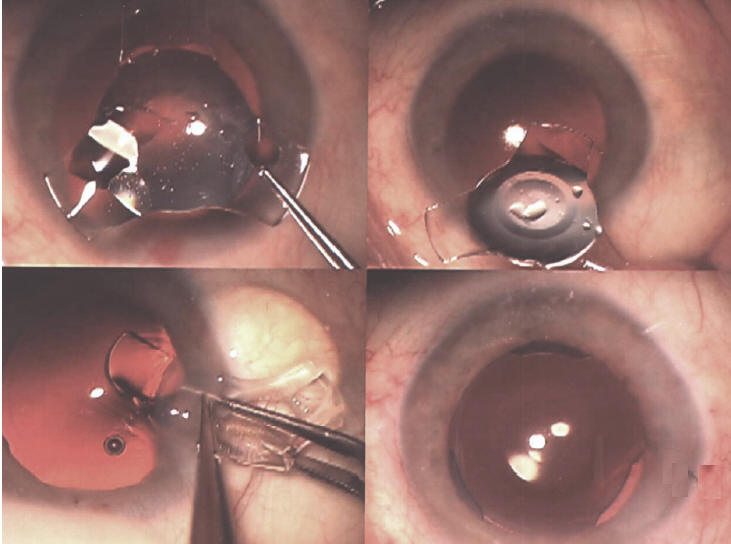
Cataract is removed through a small self sealing keyhole and there are no
sutures applied to the eye.
Todays cataract surgery practiced at Sri Venkateswara Nethralaya is stichless,
bloodless, painless procedure with a shorter overall duration of surgery. There
is very negligible postoperative discomfort with immediate restoration of
maximum possible vision usually resulting in a more satisfied patient and
surgeon in stark contrast to earlier forms of manual surgery in which a larger
incision was placed to remove the lens manually in toto and sutures were
frequently applied , which is still practiced mainly in developing countries due
to non availability of Phacoemulsification as well as non availability of
Surgeons who have mastered the art of Phacoemulsification.
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
There are various forms of intraocular lenses available for correction such as a
1.Rigid lens - That are made up of rigid PMMA material that requires a larger incision size 6mm resulting in prolonged healing time and correct the Spherical Power only.
2.Foldable lens - That are made of a foldable material and unfold inside the eye like an umbrella resulting in a smaller incision size and faster recovery and better comfort,
3.Aspheric lens - These lenses correct both spherical power as well as spherical abberation (SA) which is a higher order abberation.
We all know that the positive SA of the cornea is neutralized by the negative SA of the 19yr old lens. But as the lens progressively ages & increases its positive SA with age such that there is a residual positive SA in the aged natural optical system, the quality of vision in terms of contrast sensitivity deteriorates. However the best quality of vision is achieved in a 19yr old who has 0.0 SA while children may have residual negative SA if the optical system is taken as a whole.
Normal Prolate cornea compensates for the negative SA of the lens in large pupils producing constructive interference in normal eyes enhancing Retinal image quality and contributes towards a good OTF(Good Optical Transfer Function= Good MTF with no phase shifts) even in larger pupils of 6mm and above. Oblate corneas produce destructive interference in similar situations increasing the +ve SA in such conditions. It can also occur in virgin eyes in lenticonus etc and can appear as either positive or negative.
In normal pts, where the corneal shape is normal and SA is measured to be +ve, with or without symptoms , no history of previous refractive surgeryThe current understanding is to target a slight degree of post operative negative SA which is considered to be better than post operative positive SA. But the artificial lenses that we have been using all this while had a positive SA which added to the positive SA of the cornea which might have caused post operative HOA and night vision abnormalities. So now we have negative SA IOLs such as tecnis (0.27um) and zeiss (0.32um), Acrysof IQ (0.20um) and zero SA Iols such as Akereos sofport AO from B&L which might potentially improve night vision and contrast sensitivity. However in patients where Sa is measured to be -ve, zero Aspheric IOLs or traditional +ve SA IOLs may be preferred.
Patients with the abnormal corneal shape and large mesopic pupils with highest amounts of preop SA value as measured in OPD 11 receive a Tecnis IOL/zeiss IOL; patients with medium amounts receive an AcrySof IQ IOL; and patients with low amounts receive a SofPort AO IOL. This applies to post myopic Lasik patients with oblong corneas too where lasik would have induced positive SA in the cornea. For Post Hyperopic Lasik pts, with hyperprolate (hyper bola) corneas lasik would have induced negative corneal spherical aberration, so adding a negative SA IOL is not advised. Hence i would recommend a regular traditional+ve SA IOL if we want to neutralize the SA, or we can go for zero (SA )akreos as it is a zero SA IOL which would at least not further complicate the preop WF picture and maintain the same depth of focus.
1. The corneal shape factor or Q value is analysed to see if the aberrations have a direct correlation with the existing corneal shape or not.
Positive Q value is an area of central hyperopia followed by a ring of myopia with normalization in the far periphery after high hyperopic corrections = Sombrero hat. Negative Q value is an area of central myopia followed by a ring of hyperopia after high Myopic corrections with a normalized far periphery also called donut profile. Patient most often complain of haloe, glare, starburst, which can be overcome by pilocarpine. Some patients may complain of loss of contrast sensitivity also. For Ex, Oblate corneas (post myopic lasik) increase positive +ve SA while Hyperbola corneas (post hyperopic lasik) increase negative -ve SA. If Corneal Shape is normal, it can be presumed that other structrures like lens, vitreous etc are responsible for inducing the WF errors due to scatter, pupillary abnormalities, media opacities, poor psychophysical adaptation, cognitive abnormalities etc. If these internal errors are progressive/regressive in nature, then it is better not to correct these errors at the corneal plane permanently. Unfortunately The no abberomety map including the internal OPD map of the OPD scan does not give all of the internal aberrations. The only aberration that can be evaluated as corneal and total is SA. The difference between total SA and Corneal SA may be taken as due to internal SA. Other abberations/WF errors cannot be measured and hence we do not know if the internal SA is helping to minimize or maximize the overall HOA as a result of constructive or destructive interference.
1. Post Myopic Lasik Oblate Corneas with high +ve Total SA and -ve Q Values require IOL corrections with IOLs with negative SA while Post Hyperopic Lasik Hyperbolic Corneas with High -ve Total SA and +ve Q Values require IOL corrections with IOLs with traditional +ve SA lenses. This argument can be extended even to normal IOL power calculations where preop corneal shape and SA can be determined and IOLs customized in such a way that residual Positive/Zero SA is attained in all cases especially in large pupils.
These lenses are useful in patients with large mesopic pupils (>5mm) who exhibit large monochromatic higher order abberations which is noticeable by the average patient (as in pts with smaller pupils, the effects of monochromatic HOA's become masked by a disproportionate increase in diffraction wherein these eyes are then called diffraction limited eyes). They are useful in patients who have undergone prior hyperopic lasik (+ SA Traditional lenses are used), Prior myopic lasik ( High Negative aspheric lenses like tecnis lenses for neutralizing high + SA and moderate negative aspheric lenses like Acrysof IQ to neutralize moderate + SA are used if pt desires a high degree of spatial and temporal resolution or clarity). In normal patients and in post myopic patients who desire a greater range/ depth of vision and where tolerance to even mild defocus is suspect, zero aspheric lenses (Akreos from B & L) are used. The effects of diffraction and monochromatic HOA's tend to cancel out each other and image clarity is optimally achieved at a pupil size of 3-4 mm.
If Abnormal Q values are obtained, normally it would correlate with high WF errors in larger Pupils/Mesopic conditions. With normal Q values, WF errors may not be significant in Mesopic conditions. Any Deviations from this and the cause has to be elaborated. For Ex, Abn Q values and low WF errors, See if the Individual Zernicke Coefficients are cancelling out Each other producing a Constructive WF. If normal Q Values and having abnormal WF errors, other Causes like Tear Film abnormalities, Media Opacities, Pupillary abnormalities that may increase optical path lengths to produce destructive interference may have to be looked into. Such abnormalities need to be corrected only if they are extremely symptomatic with the patient complaining about them. Sometimes such internal abberations are progressive and it may not be a good idea to correct internal abberations in the IOL plane or the corneal plane. If low WF errors are producing symptoms ,
Ask your doctor 3 questions with respect to yourself :
1) Is the patient symptomatic w.r.t HOA? If yes and pt has large pupils , go for further investigations towards customisation of the IOL and measure the absolute HOA, if pt is not symptomatic go for zero aspheric IOL
2) Is the absolute HOA's as measured by the abberometer high? IF yes, then go for further investigations towards customisation and so, measure the Q values, if HOA's are not high then see if the zernicke modes are in the same radial order, different angular frequency or different sign. As mentioned before , if the zernicke modes are in the centre of the pyramid they tend to have a greater effect on vision than the peripheral modes even if the total WF errors are minimal.
3) Does it Correlate with abnormal Q values. If Q values are normal, HOA's are high, and pt is symptomatic then they must be internal and sometimes progressive, so be careful, correcting only the overall internal SA that too at the IOL plane may not help and may sometimes aggravate if the SA was reducing the overall HOA pre op.. If the Q values are normal, HOA's are high and pt is not symptomatic, then too one must be careful as one HOA must be cancelling out the other.
If symptoms, HOA's and Q values corelate then customization is a must.
4. Toric Lens- Correct both spherical power as well as cylindrical power and is usually made up of a foldable material. It is used if the cyl power is more than 1.5D. For powers less than 1.5, LRI's and paired clear corneal incisions are used.
5. Refractive multifocal lenses (Rezoom,Rayner)- These lenses have multiple powers arranged in concentric circles and usually provide acceptable levels of near and distance vision in a staggered pattern with objects appearing clear at some foci like 30cms/ 50cms / 75 cms/ 1mtr / 2mtr / 4mtr / 6mtr / infinity but not in a linear continuous fashion,ie in the above example, if the objects appear clear at 30cms and 50 cms, they will be blurred at 35cms, 40cms, and 45cms before they begin to appear clear at 50cms again. they do not provide a continuous spread of sharp focus over a wide range from infinity to 25cms. Zones 1.3.5 focus for distance and zones 2 & 4 focus for near. The Aspheric transition zones between these zones work for the intermediate zone.
6. Diffractive multifocal lenses (Acrysof Restor)- These lenses have Diffractive edges engraved and apodized ( step heights decrease in height from centre to periphery in a concentric fashion) that diffract or spread a larger quantity of the peripheral light rays to the distant focus when the pupil is dilated while spreading the central pencil of light rays to the near focus when the pupil is constricted. So they are dependent on the pupil size and as the pupil size is constricted due to senile miosis in elderly patients, that limits the lens from realizing its full potential in a large subsect of patients but they do provide a better spread of focus as compared to Refractive lenses in young patients with good pupillary function but they result in a loss of contrast if they are apodized ( Night vision and ability to see a white object in a white background) and usually result in good distance and intermediate vision but near vision is not satisfactory in all patients.
Non apodised lenses like the Tecnis lens from AMO have a better contrast sensitivity in some patients. Most of these lenses perform well in controlled static environments with standard lighting and illumination and a basic reading speed of 100-120 words per minute may be achieved but in terms of the reserve power required to achieve good reading speed of 180-200 words per minute in a dynamic constantly changing environment with variable depth of targetted near vision in differential lighting, most lenses perform poorly.
7. Combined Refractive and Diffractive Lens- These lenses try to mix and match the technology so that the refractive technology is infused into the front surface of the lens and the diffractive technology is engraved on the back surface of the lens. These lenses perform very well in only those patients where the preoperative Lens power calculation is perfect to the range of +/- 0.50D. The technology to calculate the Preoperative lens power with that accuracy is only 90% effective and in diseased eyes having short sight or long sight , ie that are too long or too short, the technology and formulas used to calculate lens power is only 50% accurate. This means that between 10-50% of patients will end up unhappy with the overall results while the others will be extremely happy to achieve their 19yr old vision. This creates a "all or none" effect and forces the surgeon to replace the lens with a second procedure in case of unhappy patients with another model of the lens which entails additional cost and unwanted risk.
8. Accomodating IOLs (crystalens)- these lenses change their overall shape and position depending on the amount of effort the patient (which is variable in different patients) puts in to see the near objects and although the quality of distance vision is good, the near vision is not upto the mark in patients who may not be able to put in the required effort.,
9. Presbyopia Lenses with Enhanced depth of Focus (EDF) such as Tecnis Symfony lens are a different group altogether where they correct chromatic abberation too along with spherical power, spherical abberation and cylindrical power if present. Theoretically, they can help the patient acheive 20/10 vision. Hence the strategy is to make the patient a residual myope of -0.75D to -1.0D so that he can acheive a near vision of N6 while a distance vision of 20/20 is acheived. Although These lenses can technically allow the patient to achieve 20/20 vision along with N6 vision . They are useful in mild myopes, unilateral cataracts, and fellow eye of patients who have undergone cataract surgery before with monofocal IOL and would like to have some amount of near vision too in the current procedure. However in those patients who have residual power as a post op surprise, they do not require additional surgery and lens removal again and a simple pair of additional single vision glasses may be sufficient to achieve good distance, near and intermediate vision.
As you can see, each of the above lens designs have a few advantages over the other in that order. As these lenses will serve you for the rest of your life, it is important that we choose the lens that will provide the best spatial resolution/clarity to 2 dimensional static images as well as temporal high definition quality to kinetic 3 dimensional moving/mobile imagery. It is also important that the lens selected conforms to your visual needs and demands.
Your eye surgeon will determine the type of lens best suited for you depending on the general health of the eye. Sometimes a mix and match strategy may be applied where the dominant eye may get a lens which is expected to work very well for distance and intermediate zones while the non dominant fellow eye may get a lens which is expected is work very well for distance and near.
Although all these lenses will get locked into their position for the rest of the patients life inside the eyeball, it does not necessarily mean that they will continue to function the same way year after year. Some patients may have or develop in future retinal disorders like Macular Degeneration, Central Serous Retinopathy etc, where some of these lenses will not work very well. Some patients may have predisposing factors which places them at a risk of developing future retinal problems and eye surgeons then try and avoid some of these lenses in such patients too.
Basic Rigid IOLs are not very expensive and the total package cost for surgery with these IOLs ranges from Rs 15000 to Rs 20000. These IOLs will provide acceptable levels of distance vision without glasses, but for fine vision, one has to wear glasses both for distance and near.
Premium lenses are lenses other than basic IOLs and have additional features that can augment, support and reinforce other vision related qualities so that the overall visual experience is seamless. The foldable nature of the lens provides a high degree of postoperative comfort and faster recovery, The Asphericity provides superior night vision capabilities as well as enhanced spatial and temporal resolution. Correction of cyl power by Toric IOLs minimises the residual power postoperatively and customisation can be done on Post op WTR or ATR depending on whether the pt desires better range or better clarity and reading speeds at a given near focal point.
MULTIFOCAL LENSES allow the patient to see normally both for distance as will as
near and intermediate distances without glasses and are usually the best lenses
used worldwide for visual restoration. SVN has tied up with Carl Zeiss
Meditec and AMO to offer Acritec Multifocal IOL and Tecnis Multifocal IOL to
our patients. These Lenses are expensive and the
total surgical cost varies from Rs 75000- Rs 1,10,000 depending on the type of the IntraOcular Lens used. These Refractive and diffractive IOLs provide
simultaneous distance, near and intermediate vision and currently are widely
used in western countries although the uptake in India is still negligible due
to the cost. These IOLs too are offered at Sri Venkateshwara Nethralaya for
patients who desire a greater degree of independence from glasses.
SVN has also tied up with Bausch & Lomb to offer Crystalens AO, Crystalens HD, and Crystalens Five-O to its patients. This IntraOcular lens is a accomodating IOL that provides acceptable levels of Distance, near and intermediate vision but with a greater degree of Contrast Sensitivity as compared to even Multifocal IOLs, So patients who choose Crystalens can expect greater degree of freedom from Glasses as well as greater Night Vision due to better contrast sensitivity. However this IOL is very Expensive and the package rates vary from Rs 1.3 Lakh to Rs 1.5 Lakh per eye. Not every one is a candidate for these lenses and you will have to enquire with us whether you are a eligible candidate for these lenses.




